SOCIALISM FOR THEM: 60% of Anthem’s 2021 revenue was subsidized by American taxpayers.
As the company’s profits have soared, courtesy of America taxpayers, so have Americans’ deductibles.
When I was growing up, it seemed that everybody who had health insurance had a Blue Cross plan.
Every state had a Blues plan, every one of them was a nonprofit, and their policies were comparatively cheap and comprehensive.
That seems downright quaint when you consider what has happened to the Blues as more and more of them, starting in 1992 with Blue Cross of California, began to ditch their nonprofit status. Many of them, including the giant Blue Cross of California, are now owned by an Indianapolis-based corporation that has grown to be the second largest in the industry in terms of health plan membership. It is also one of the most profitable.
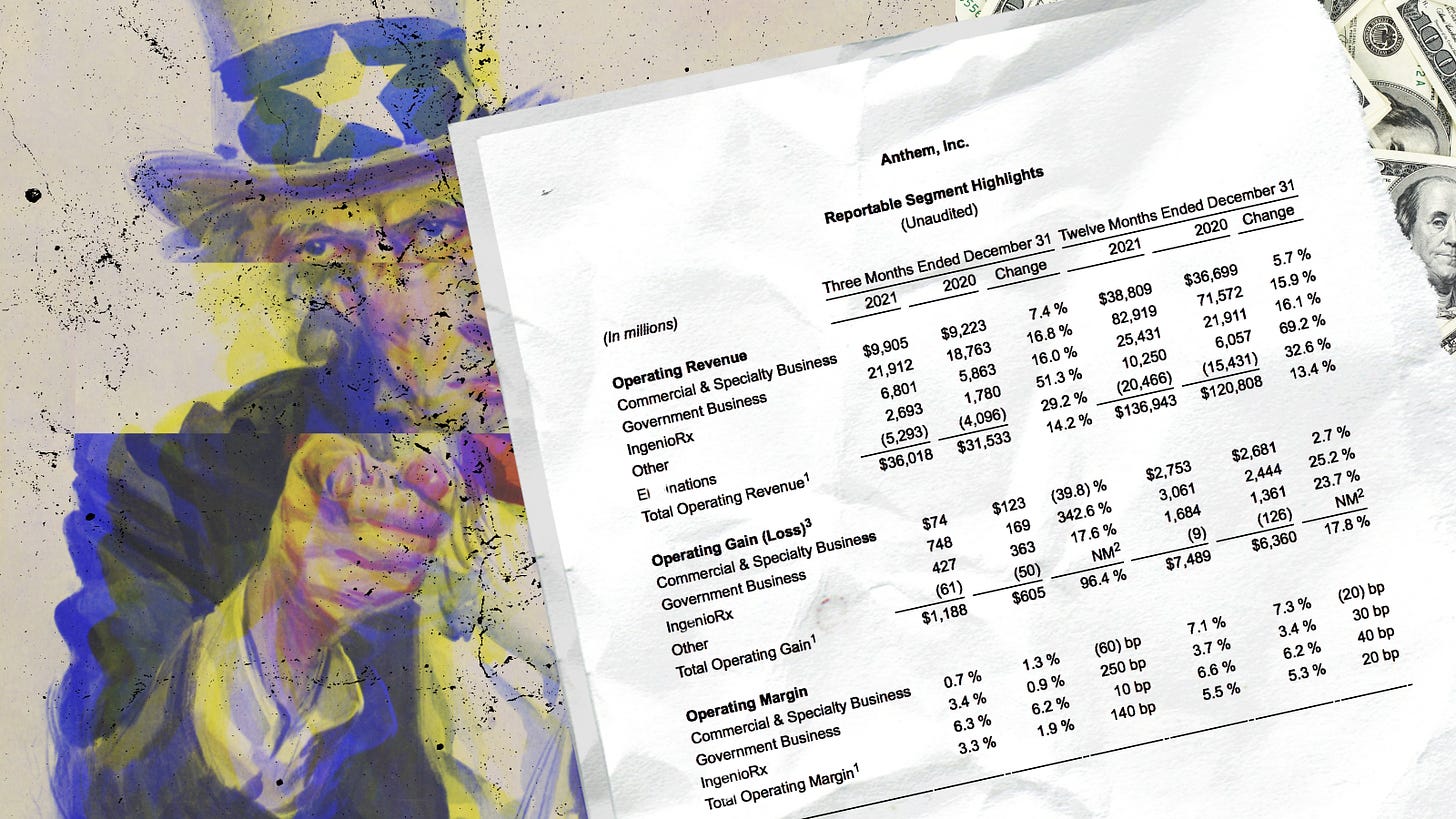
That company, Anthem, Inc., which operates Blues plans in 15 states, reported last Wednesday that it’s 2021 profits totaled $6.1 billion on revenues of $136.9 billion. That’s more than twice the $2.6 billion in profits the company reported making 10 years ago (when the company was still known as WellPoint, Inc.).
When I was a kid, many if not most folks, including my parents, bought their Blue Cross policies on their own, without any financial assistance from an employer (or the government for that matter). Relatively few employers back then, especially in rural areas and small towns, offered subsidized coverage to their workers. And to my knowledge, the Blues didn’t have anyone anywhere covered in a health plan subsidized by taxpayers.
(That began to change in the 1980s when President Reagan and Congressional Republicans began what would be a years-long and increasingly successful effort to privatize the Medicare program. Privatization of Medicaid began a few years later when states began contracting with private insurers to manage their taxpayer-financed health insurance program for low-income individuals and families. My home state of Tennessee was among the first to do that when it created TennCare in 1994 and tapped Blue Cross Blue Shield of Tennessee to administer it.)
What a difference a few decades can make. When you look closely at the numbers Anthem disclosed last week, you’ll discover that 61% of the company’s nearly $137 billion in revenues came from the government–or more precisely, from the federal and state taxes you and I paid last year.
(That 61% figure doesn’t really capture all the money Anthem takes in from taxpayers. If you factor in the subsidies most people enrolled in Anthem’s ACA marketplace plans are receiving to help them pay for premiums they otherwise couldn’t afford, the percentage of the company’s revenues coming from taxpayers undoubtedly would be even higher. Anthem doesn’t provide enough granularity to determine a precise number.)
When Anthem briefed analysts and investors last Wednesday about its 2021 profits–which were higher than even Wall Street financial analysts had expected–the company’s executives noted that more than 45 million people were enrolled in Anthem’s health plans at the end of the year, up 2.5 million from 2020. That is impressive growth, for sure. But when you examine Anthem’s health plan enrollment numbers, you’ll see that all but about 250,000 were people newly enrolled in Anthem's Medicare Advantage plans and, especially, in the Medicaid programs Anthem manages for several states.
Like UnitedHealth, which I wrote about last week, almost all of Anthem’s growth is now at the expense of taxpayers, not from growth in its commercial book of business, which not so long ago was Blues plans’ only book of business.
When you compare Anthem’s 2011 and 2021 financial disclosures, you’ll see that 90% of Anthem’s membership growth over those 10 years was in its Medicaid and Medicare business. Of the 11.1 million additional people who enrolled in Anthem’s health plans between 2011 and 2021, 10.1 million were new Medicaid and Medicare enrollees. But unlike United, Anthem’s growth came mostly from its Medicaid business. United’s growth was fueled primarily by its AARP-affiliated Medicare Advantage operations.
Anthem has been a favorite of Wall Street analysts and investors over the past decade, despite its anemic commercial business and its growing dependence on Uncle Sam for its profitable growth. Between December 30, 2011 and December 31, 2021, Anthem’s share price increased more than 800%, from $56.80 a share to $463.84 a share. In 2021 alone, Anthem’s market capitalization swelled 43%, from $78.8 billion on December 31, 2020 to $112.5 billion on December 31, 2021.
Investors have made enormous gains not only as their Anthem stock has increased in value (if you’d invested $130,000 in Anthem’s shares at the end of 2011, you’d be a millionaire today) but also through the company’s dividend and share repurchase programs. During the final three months of 2021, as American families’ premiums and deductibles continued to increase, Anthem distributed $274 million in dividends to shareholders and spent $522 million buying back shares of its own stock (almost $2 billion over the course of last year and billions more than that over the past several years).
While Anthem was rewarding its shareholders so handsomely over the past decade, the average cost of an employer-sponsored family policy increased 47%, from $15,073 in 2011 to $22,221 in 2021, much faster than average wage growth and household income (unless, of course, you were an Anthem shareholder).
Meanwhile, premiums and deductibles have grown to consume more than 10% of family household budgets in 37 states (including all but three of Anthem’s 15 states), up from 10 states 10 years ago. In many states where Anthem owns a Blues plan (California, Colorado, Connecticut, Georgia, Indiana, Kentucky, Maine, Missouri, Nevada, New Hampshire, New York, Ohio, Virginia and Wisconsin) deductibles alone have increased more than 200% over the past decade.
Even with all the money Anthem is taking in from taxpayers, more and more families enrolled in Anthem’s commercial health plan are being pushed into the ranks of the underinsured–and in many cases into bankruptcy when a family member gets sick. Unlike Anthem’s wealthy shareholders, fewer and fewer families have enough money in the bank to meet their ever-growing out-of-pocket requirements before their health insurance coverage kicks in. That means that Anthem can avoid paying millions of medical claims. No wonder the company is a Wall Street favorite.
(An historical side note: There has arguably been at least one upside to the greed of Anthem’s executives. Back in 2009, just as support was waning for legislation that would eventually become the Affordable Care Act, Angela Braly, the company’s CEO at the time, insisted that Blue Cross of California increase premiums for its individual insurance policies an average of 25%, with some rates going up as much as 39%. Congressional Democrats were so outraged when they caught wind of it they hauled Braley before the House Energy and Commerce Committee. It did not go well for her. Democrats got the bill across the finish line a few weeks later in March 2010. Two years after that, Braly was forced to resign when it was investors’ turn to get outraged, not because of rate increases but because they weren’t happy with the company’s second quarter profits. Still, Braly got a big raise that year and walked away with more than $20 million in her pocket.)



just when you think things can't get more disgusting......
I want to fix the misspelling of "courtesy" in your subhed because you are reporting important things.